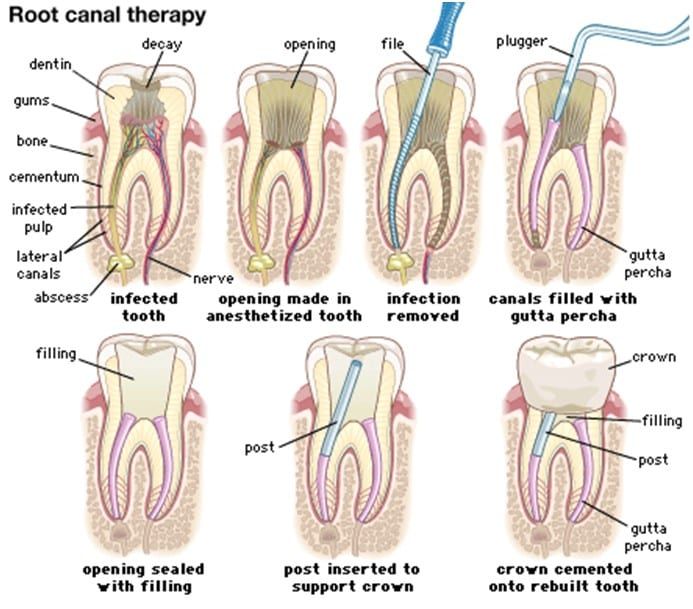
What goes beyond the root canal? Because root canals need to have ample tooth supply to have a chance at being saved, people who have tooth fractures beyond repair and deteriorating teeth and those who have highly infectious dental pulp can spread throughout the bloodstream, thus requiring surgery. Root canals are considered nonsurgical procedures, even with the tooth’s root channels’ removal and fillings. But for those who aren’t able to qualify for a root canal, the next step recommended is endodontic surgery.
What is Endodontic Surgery?
Endodontic surgery works to locate small, hidden fractures that are undetected by x-rays during the initial treatment. Most often, when a general or family dentist is unable to resolve the tooth pain, or when the tooth trauma is so severe that their tools and expertise is unable to address the issue, or when there are signs of a tooth pulp infection that cannot be treated through generic antibiotics. Endodontists specialize in the form of surgery that specifically works within the endometrium, or the section of the tooth hidden internally containing the pulp, root canals, dentin, and roots.
Endodontic surgery encompasses many traits, and endodontists work within this specialty to provide patients with additional options for tooth repair and restoration. Digital imaging, operating microscopes, and microscopic tools are used during this form of surgery to treat various conditions that your general dentist may not be able to treat, including:
- Microscopic cracks in the roots
- Persistent cysts beneath the gum line
- Blocked root tips caused by calcium deposits
- Abnormal formations in the root canal channels
- Necrotic or damaged pulp
Endodontic surgery can also diagnose symptoms related to tooth pain that cannot be detected through nonsurgical treatment. Reoccurring infections even after a performed root canal procedure may also require endodontic surgery, like those rare cases where reinfection occurs will require further analysis. Endodontists work to preserve the inner tooth by bringing advanced techniques to the forefront of dentistry and use these techniques to provide people with long-term, substantial relief:
- Endodontic Retreatment: This procedure involves removing the previous crown and material, cleaning the infected root canals, and repackaging the root channels with new material and a new crown.
- Dental Implants: When the tooth’s unable to be saved by endodontic surgery, tooth extraction is performed and then replaced with a dental implant to restore the tooth.
- Calcium Removal: Often, if the root canal is blocked by heavy amounts of calcium deposits, then an endodontist would need to remove those deposits to prepare the tooth for a root canal.
- Endodontic Examinations: If your general dentist cannot identify acute pain, then an endodontic examination using surgical techniques will be administered to diagnose the problem.
- Pulpotomy: Pulpotomies remove the pulp and remove the pulp within the crown section of the tooth, leaving the pulp in the root channels intact. This procedure is mainly performed for children’s primary teeth.
- Pulpectomies: A pulpectomy completely removes the pulp from both the crown and the root canal and is mainly performed on children’s primary teeth to remove the infection.
Most commonly, however, apicoectomies are performed when root canals cannot achieve the results needed to sustain the tooth’s internal structure and integrity.
What is Apicoectomy?
Apicoectomies work to remove the infected pulp beyond the tooth’s roots and into the jawbone and help heal the roots by re-sectioning them back into place. This microscopic surgical procedure is often used when a root canal treatment doesn’t provide the patient with pain relief or when the root canal is unable to completely remove the infected pulp.
Apicoectomies remove the tip of the root that’s connected to the integral jawbone, called the apex. The apex features openings for the blood, nerves, and lymph vessels to enter the pulp. In general, the apex can lead into accessory canals that branch out throughout the tooth, intermixed with dentin and cementum. The apex and its channels help connect the tooth to its surrounding gum tissue and jawbone material. When the pulp is infected, it can spread to the apex and surrounding gums and cause the blood and nerve vessels within the tooth the die-off.
Apicoectomies often have to go beyond the apex and into the underlying bone to remove the pulp that has been left behind and severely damaged, and then fill the area with a sealant to protect the area from future infections. Like root canals, apicoectomies are advanced forms of root canal procedures that work within a different area of the tooth’s anatomy to help patients find better pain relief.
When is an Apicoectomy Needed?
This type of surgery is often needed for those who have had some sort of failure with their root canal procedure, where the underlying cause of the root pain was either unaddressed or un-diagnosed. This surgery is meant to help patients save their tooth if their tooth still has a healthy tooth structure and can be repaired through restorations. The best way to determine if an apicoectomy is required is to speak with your primary dentist about your tooth pain and what options you have available according to your condition. In general, endodontists perform apicoectomies when these conditions are present:
- Apical Periodontitis – Inflammation of the periodontium, or gum tissue area, that’s sourced from an infected pulp at the apex of the tooth will often require an apicoectomy when the pulp infection has spread so severely that it’s begun to seep into the jawbone material.
- Irreversible Pulpitis – Inflammation of the inner pulp that causes apical periodontitis conditions will require apicoectomies if the infection is at its chronic stages.
- Advanced Pulp Necrosis – Pulp tissue dying within the apex can lead to severe infection that spreads throughout the jawbone will often require an apicoectomy to treat.
- Failed Root Canal Treatments – If all of the above conditions don’t resolve with a root canal treatment, then an apicoectomy is necessary.
These conditions can be caused by various factors, including cavities, tooth trauma, and improper restorative treatment. Endodontists often need to determine whether or not an apicoectomy is necessary based on factors related to the tooth’s internal structure. If it cannot be saved, then a tooth extraction and restoration would need to be performed.
For more information about apicoectomies, how to prepare for your surgical procedure, and what procedures would be used during your surgery to correct your tooth pain, contact your primary dentist or endodontist to gain more about endodontic treatment.