Beyond handling dental emergencies and performing root canals, endodontists have other nonsurgical and surgical methods for saving teeth. However, there is an ethical and moral responsibility placed on dentists and endodontists to provide treatments in the best interest of their patients. As endodontists, we face challenges daily regarding our patients, especially when cases appear simple but ultimately become more complex over time as new information is learned. However, dentistry’s fast pace production has led many to avoid providing services that have their patient’s best interest at heart. When facing these challenges, it also comes with an understanding of what’s appropriate and what isn’t for treatment.
Endodontic retreatments have been discussed through numerous evidence-based studies and compared to more surgical means, such as extractions and implants, to help dentists further understand what treatments are most appropriate for their patients. Through this article, we will be discussing the various circumstances surrounding these treatment methods, how they impact our patients, and how to better optimize clinical success for future treatments.
What is Endodontic Retreatment?
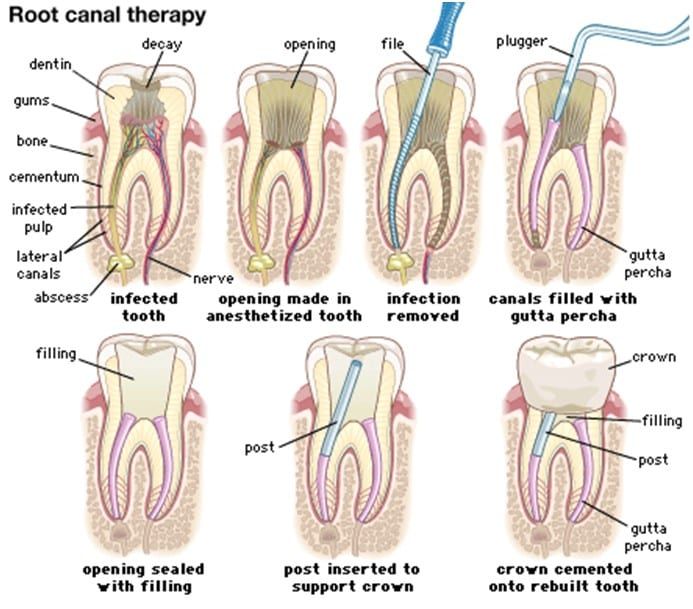
Root canal treatments are meant to last the patient’s lifetime, but in some cases, teeth suffering from more complex cases of tooth fractures, apical periodontal disease, and overfilled tooth canals can ultimately face more problems than they originally had. In cases where these failures occur, endodontic retreatment is needed to correct those issues. Often, endodontic failure mostly occurs due to the presence of bacteria throughout the canal system or the periodontal ligaments. Retreatment often works to remove this bacteria, and retreatments are most often performed nonsurgically, using obturation techniques to access the canal and endometrium areas and remove the bacteria present.
But one of the assessments most often made by endodontists in these circumstances is knowing when retreatments are necessary. Nonsurgical retreatments offer a 95% success rate for patients under normal circumstances. However, issues that arise during the retreatment process, including complex restoration problems, restoration posts, and other issues, can present challenges when attempting retreatments, often leading to inadequate access. To further expand on this subject, we would also need to look at the next steps, which include endodontic surgery, tooth extraction, and implants.
Endodontic Surgery, Extraction, and Implants
Large restoration removals, inability to use instruments to access the root canal, and failed transported canals can make endodontic retreatment impossible, and endodontic surgery would be considered the next step. Endodontic surgery isn’t meant to address the entire canal system but rather works with surgical techniques to work within at least 6mm of the canal system. The 6mm through the canal system is often where most bacterial infections reside, and endodontic surgery can help irrigate and remove bacteria through irrigation methods.
Endodontic surgery presents the next steps when retreatment doesn’t meet the needs of the patient. However, endodontic surgery most often works when those complex issues, such as restoration issues and moderate bacterial infection, can be bypassed easily. Post-treatment endodontic disease, though, is an unfortunate factor that often results in extraction and implants and presents an unfortunate reality for many patients.
So, how does an endodontist decide on their form of treatment? All factors related to their patient’s treatment rely on the patient’s current health of the teeth, what can be observed from the affected tooth, and the observations made by the endodontist to help maximize clinical healing. In this regard, it’s all about natural retention, and when it comes to maintaining that natural retention, the main goal is to conserve the natural tooth as much as possible.
Solving Complex Dental Problems and Their Treatments
Endodontists working with the patient in mind will often have to consider various factors, reliant on both the patient’s experience and their clinical findings, to diagnose and treat the affected tooth. We’re going to outline here some of the more complex cases often found in endodontics, specifically after a failed root canal treatment, and address the appropriate treatments:
- Post-Treatment Endodontic Disease: Post-treatment endodontic disease, referred to also as periradicular lesions, is when a previous root canal treatment fails and the root-filled tooth can no longer undergo the healing process necessary. Foreign material throughout the periapical area and micro-organisms often can cause an inflammatory reaction that allows the presence of bacteria to continue growing, causing the initial root canal to falter. In these cases, both endodontic surgery and extraction and implants can address the issue, but most often, extractions and implants have more long-term success rates than endodontic surgery.
- Vertical Fractures: Vertical fractures throughout the tooth, whether appearing in the apex of the tooth and then extending towards the coronal area, highly threaten the tooth’s lifespan. Through the appearance of vertical fractures, the root channels develop depressions, the dentin layer decreases, and higher amounts of corrosion from posts and pins. Ultimately, endodontic surgery to realign pins, remove excess dentin layer, and in other cases, retreatment may also be used to access the root structure and shapen the canal space.
- “True” and “Bay” Apical Cysts: Apical periodontitis can occur before root canal treatment and after root canal treatment, and these cysts often contain bacteria that cause severe inflammation along the root canal and are often associated with intra-radicular endodontic infections. In these cases, endodontic surgery or extractions and implants would be the preferred solutions, depending on the progression of the cysts concerning the damaged tooth.
Why Combined Methods Can Work Best For Endodontic Treatment
Ultimately, some cases won’t only just require nonsurgical treatment, especially when there are persistent infections, insufficient restorations, and microscopic vertical fractures present. Our goals as endodontists are to determine the overall cause of failure resulting from the previous root canal treatment, and in many cases, combined approaches provide the most applicable solutions. By removing the bacteria etiology present within the affected tooth and then providing a complete coronal seal, endodontic retreatments and endodontic surgery can allow patients to maintain their teeth. In contrast, extractions and implants allow for more long-term solutions to complex dental problems that cannot be fixed by conservative treatments alone.